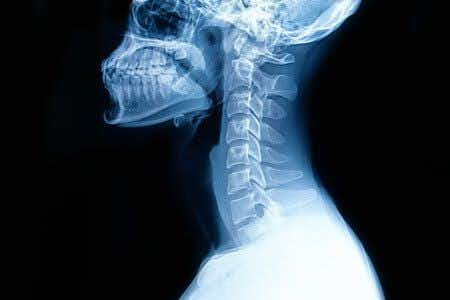
This case takes place in Missouri and involves a female patient who underwent fusion surgery on her upper spine. The patient was discharged but later returned to the ER with signs of sepsis from the surgical site, and was consequently was admitted to the ICU. A scan of the upper spine did not reveal evidence of an infection or any other damage to the spine. However, it did not rule out damage at another level of the spine, and did not explain the patient’s symptoms. Some time after initial presentation, the patient developed numbness in her lower extremities. The treating surgeon was notified but did not order any emergency investigations or imaging. Later that day, another scan of the upper spine was ordered as a non-emergency. Upon review of the upper spine, there were no signs of any abscesses. Some time later, another scan of the lower spine was conducted which revealed an infection and several other issues. The patient was taken to the OR for immediate surgical treatment. The remainder of the patient’s admission was difficult, and she never regained motor function in her legs.
Question(s) For Expert Witness
1.) Do you have experience treating spinal cord compression, resulting from infection? If so, how often?
2.) Should an MRI of the entire spine have been ordered when the patient initially presented?
Expert Witness Response E-007133
I treat patients with spinal infections, epidural abscess and spinal cord injuries. In a given year, I estimate that I have to decompress the spinal cord for an infection between 10-30 times. I estimate that I treat 2-3x that many patients/year with spinal infections, but most do not require surgery. With the clinical scenario presented to me, I would have ordered a cervical MRI especially with a draining surgical wound. If the cervical MRI was negative for infection, and another obvious source of infection had not been determined for the patient's symptoms, I would have ordered a thoracic/lumbar MRI.
About the author
Joseph O'Neill
Joe has extensive experience in online journalism and technical writing across a range of legal topics, including personal injury, meidcal malpractice, mass torts, consumer litigation, commercial litigation, and more. Joe spent close to six years working at Expert Institute, finishing up his role here as Director of Marketing. He has considerable knowledge across an array of legal topics pertaining to expert witnesses. Currently, Joe servces as Owner and Demand Generation Consultant at LightSail Consulting.