This case involves a forty-one-year-old female who presented to the emergency room at the request of her primary care physician for severe persistent headaches. CT head reports were normal and a lumbar puncture was also negative, however initial blood work revealed an elevated white count (26.3) and abnormal liver enzymes. Despite the derangement in lab values, the patient was discharged home from the ER without any further intervention. EMS was called to her house the following evening where medics found the patient to be unresponsive; she was rushed back to the hospital, intubated, and treated for what was thought to be septic shock. The patient was treated in the ICU and various consults were called, infectious Disease and G.I. recommendations, but the situation deteriorated rapidly and the patient died shortly thereafter.
Question(s) For Expert Witness
1. What would the proper course of action be in this case?
Expert Witness Response
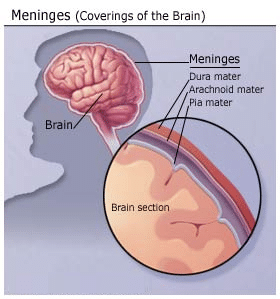
Meningitis is an inflammatory disease of the leptomeninges, the tissues surrounding the brain and spinal cord, and is defined by an abnormal number of white blood cells in the cerebrospinal fluid (CSF). Routine blood work is often unrevealing. The white blood cell count is usually elevated, with a shift toward immature forms; however, severe infection can be associated with leukopenia. The platelet count may also be reduced. Leukopenia, elevated liver enzymes, and thrombocytopenia have correlated with a poor outcome in patients with bacterial meningitis. Patients with these abnormalities should be admitted for observation for twenty-four hours.
About the author
Dr. Faiza Jibril
Dr. Faiza Jibril has extensive clinical experience ranging from primary care in the United Kingdom, to pediatrics and child abuse prevention at Mount Sinai Hospital, to obstetrics in Cape Town, South Africa. Her post-graduate education centered on clinical research and medical ethics. Dr. Jibril is currently Head of Sales in the US and Canada for Chambers and Partners - a world leading legal ranking and insights intelligence company.