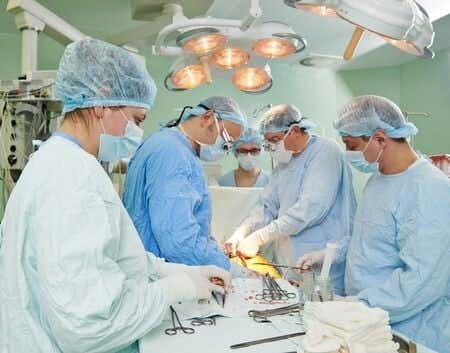
This case involves a middle-aged female who presented to a breast surgeon with an existing diagnosis of breast cancer. At the time of presentation, the physician recommended a treatment plan of chemotherapy followed by surgery. The patient was offered and agreed to total mastectomies of both breasts, to be undertaken after she completed chemotherapy. After the patient’s regimen of chemotherapy was completed, imaging reported an excellent result and the patient underwent surgery. Following the surgery, the Defendant physician informed the patient that a full biopsy would be done. The biopsy performed revealed metastatic carcinoma involving a number of lymph nodes. The Defendant told the Plaintiff that she did not need additional surgery, citing “recent literature” that claimed identical survival rates for patients who received only external beam radiation compared with those who received both surgery and radiation. Eventually, the patient received a second opinion and was told that she needed to have surgery immediately.
Question(s) For Expert Witness
1. Do you routinely treat patients with the presentation described above?
2. Could this patient's lymph nodes have been removed in a more timely manner rather than relying solely upon radiation therapy?
3. Is it likely that the delay would impact this patients prognosis?
Expert Witness Response E-000029
The issues in this case are mostly controversial. A repeat axillary node biopsy after a sentinel node was questionable and should not have been done, but an axillary dissection should have been carried out, but accuracy of a biopsy in such situations is low to poor. The wait for the biopsy may have accounted for additional delay. Whether radiation should be used or axillary dissection is in a current clinical trial, so it is not known if the patient's lymph nodes could have been removed in a more timely manner. There is an ongoing randomized trial that specifically addresses axillary management following neoadjuvant chemotherapy in patients with proven axillary node metastases. If the sentinel nodes remain positive after neaodjuvant chemo, Alliance A11202 randomly assigns patients to axillary dissection vs no axillary dissection with nodal radiotherapy for all patients. Patients received neoadjuvant chemotherapy followed by sentinel lymph node biopsy. This means that both options are clinically acceptable at this time.
About the author
Joseph O'Neill
Joe has extensive experience in online journalism and technical writing across a range of legal topics, including personal injury, meidcal malpractice, mass torts, consumer litigation, commercial litigation, and more. Joe spent close to six years working at Expert Institute, finishing up his role here as Director of Marketing. He has considerable knowledge across an array of legal topics pertaining to expert witnesses. Currently, Joe servces as Owner and Demand Generation Consultant at LightSail Consulting.