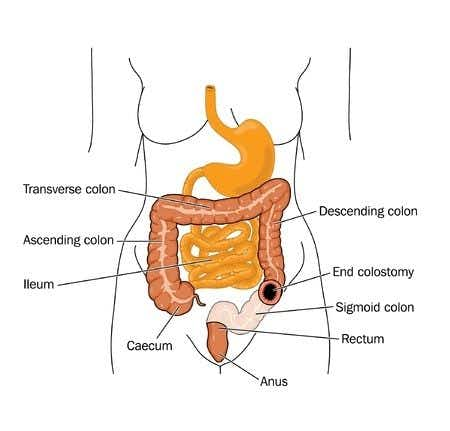
A general surgery expert witness advises on a case happened in Delaware involving a sixty-one year-old male patient with a past medical history of ischemic bowel disease. He presented to an urgent care facility at 1PM with complaints of severe abdominal pain and discomfort. The patient reported that the onset of the pain was about 2 hours earlier and was associated with chills, dry heaves and radiated from the suprapubic/bilateral lower quadrant. The patient described the pain as 10/10 and he had only 1 small bowel movement during the days leading up to this incident, which he described as extremely hard and solid. The patient was discharged by the physician with a diagnosis of constipation and was prescribed Colyte and instructed to take Vicodin for relief. Approximately 3 hours later, the patient presented for a 2nd visit to the urgent care facility where a similarly limited workup was ordered. The patient was discharged quickly and advised to get rest and take Vicodin for relief. Finally, approximately 4 hours later, the patient presented for a 3rd visit to the facility and was promptly referred for ER workup, at which point an exploratory laparotomy was performed. The patient required a significant resection of the sigmoid, descending, transverse, ascending and cecum portions of the colon. Approximately 50 percent of the distal small intestine was resected and the patient now requires a colostomy bag. The size of the hole identified in the patient’s sigmoid colon was approximately 2 inches in a linear basis and stool was exiting the colon into the peritoneal cavity at the time of the surgical procedure.
Question(s) For Expert Witness
1. Do you routinely perform the surgical procedures described above?
2. Could earlier intervention have made a difference to the outcome for this patient?
3. Have you ever served as an expert witness on a case similar to the one described above?
Expert Witness Response E-001161
I take a lot of acute care surgery calls, so I do see ischemic colitis consults often. I do perform colon resections as well, mostly for diverticulitis and its associated complications. Most of the elective colon cases (ie, cancers) are handled by the colorectal surgeons on staff. In addition, I see a fair number of mesenteric (or small bowel) ischemia consults. As for the case above, it is definitely odd how a patient with a known history of ischemic colitis could present to an urgent care facility with acute abdominal pain and not have any imaging. It looks like he had a pretty extensive resection of both his colon and small bowel. In regards to acute ischemia, timing is everything. The goal is to reverse the ischemia within several hours of onset, otherwise the bowel will most likely not be salvageable (it will be necrotic and need to be resected). So earlier intervention in this patient would have likely led to less bowel being resected and possibly less contamination from stool spillage. This patient warranted a more thorough evaluation by the clinician, including CT scan and blood work. Undoubtedly, the workup would have shown that he was septic, and required surgery. The diagnosis of "constipation" is one of exclusion, only to be made after other diagnoses of ischemia, colitis, diverticulitis, or intra-abdominal sepsis has been ruled out. It sounds as though he was inappropriately evaluated, and a timely diagnosis may have saved him from an extensive operation.
About the author
Dr. Faiza Jibril
Dr. Faiza Jibril has extensive clinical experience ranging from primary care in the United Kingdom, to pediatrics and child abuse prevention at Mount Sinai Hospital, to obstetrics in Cape Town, South Africa. Her post-graduate education centered on clinical research and medical ethics. Dr. Jibril is currently Head of Sales in the US and Canada for Chambers and Partners - a world leading legal ranking and insights intelligence company.