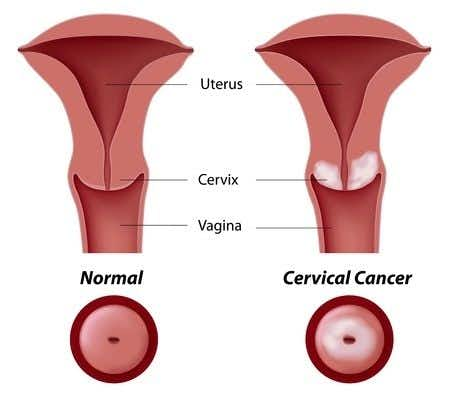
In 2001, decedent’s Pap smear results indicated a low-grade squamous intraepithelial lesion. Her obstetrician ordered a colposcopy and an endocervical curettage, which were both normal. A few months later, another Pap smear reported as atypical squamous cells of undetermined significance/favor dysplastic process. Four years later, she had an HPV test that was reported to be positive for high-risk strains of HPV. She was diagnosed by biopsy with in situ squamous cell carcinoma of the labia. This was surgically removed. A colposcopy of decedent’s cervix was normal. Two years later, a left labial biopsy was positive for mild squamous dysplasia
A few months later, in 2008, decedent became a new patient of the defendant doctor. She did not inform him about her prior abnormal Pap smears, HPV risk or treatment for vulvar dysplasia. The defendant performed a Pap smear that was analyzed by defendant laboratory and found to be normal. A year later, decedent saw defendant’s partner, who diagnosed her with vulvovaginitis. No Pap smear was performed. The following year, she went to another gynecologist, who found a 3-4 cm exophytic mass protruding from her cervix. She was diagnosed with clear cell adenocarcinoma of the cervix and underwent a complete hysterectomy. A year later, she was diagnosed with squamous cell cancer and she died within six months.
Decedent’s representative alleges the laboratory, located in Virginia, failed to detect cells that would have led to early treatment for the cancer.
Question(s) For Expert Witness
1. Did the interpretation of the Pap smear delay decedent’s treatment?
2. Was her cancer typical?
3. Was anyone else negligent in her treatment?
Expert Witness Response
Decedent’s disease status in 2008 is unknowable. Even assuming her 2008 Pap smear indicated cells that could be interpreted as suggestive of a high-grade lesion (HSIL), which I cannot independently assess, the Pap smear is non-diagnostic. In other words, even if her 2008 Pap smear was interpreted as HSIL, it indicates only that further investigation of her actual condition was warranted-not that she had dysplasia. In short, the only reliable method of determining whether and to what degree the decedent had cancer or pre-cancer in 2008 would be through biopsy of the affected area, and one was not performed at that time. Similarly, there is no other medical evidence from around the time of the 2008 Pap smear that suggests she had cancer or pre-cancerous dysplasia, such as other positive Pap smears, suspicious findings on physical examinations or imaging studies, or the like. Moreover, she had a grossly normal pelvic exam in February 2010, just eight months before she was diagnosed with a visible 4 cm lesion in her cervix.
The evidence suggests the disease developed close to the date it was definitively diagnosed in October 2010, probably after the 2008 Pap smear, and spread rapidly. All that really can be said is that her disease was rapidly progressive (got much worse over a relatively short period of time), but one cannot reliably predict when it started, or when it passed a point at which, for decedent, it could not be successfully treated.
Further, the defendant doctor and his partner breached the standard of care by not obtaining complete medical information from decedent and in not ordering additional testing when she finally did report her prior diagnoses and treatments. For the same reasons, it is my opinion that the decedent was also negligent or acted unreasonably under the circumstances by not having a Pap smear in 2007 or 2009 or providing an accurate medical history.
The expert is a gynecologic oncologist and professor who has been in practice for 25 years.
About the author
Kristin Casler
Kristin Casler is a seasoned legal writer and journalist with an extensive background in litigation news coverage. For 17 years, she served as the editor for LexisNexis Mealey’s litigation news monitor, a role that positioned her at the forefront of reporting on pivotal legal developments. Her expertise includes covering cases related to the Supreme Court's expert admissibility ruling in Daubert v. Merrell Dow Pharmaceuticals Inc., a critical area in both civil and criminal litigation concerning the challenges of 'junk science' testimony.
Kristin's work primarily involves reporting on a diverse range of legal subjects, with particular emphasis on cases in asbestos litigation, insurance, personal injury, antitrust, mortgage lending, and testimony issues in conviction cases. Her contributions as a journalist have been instrumental in providing in-depth, informed analysis on the evolving landscape of these complex legal areas. Her ability to dissect and communicate intricate legal proceedings and rulings makes her a valuable resource in the legal journalism field.