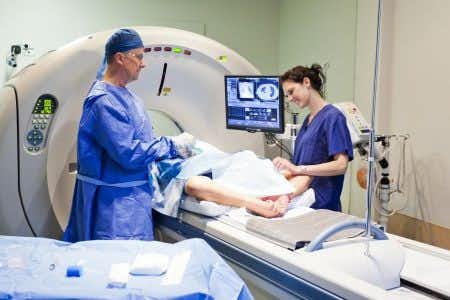
This case involves a sixty-year-old male patient who presented to the emergency room complaining of a six day history of neck pain radiating to his back and right shoulder. During a series of visits back-and-forth between the emergency room and his primary care doctor, no abnormalities were found on chest x-ray, shoulder x-ray, EKG, and MRI. He returned again to his primary care physician with the same complaints of severe pain in his neck and right shoulder. The pain had now extended to his right arm. The patient’s wife, who accompanied him to the doctor’s office, reported that he had been feeling disoriented at times and was experiencing a burning sensation while voiding. The primary care physician suspected that the patient was suffering from prostatitis and prescribed a course of Ciprofloxacin. The patient was compliant and took the medication as advised. However, he was an avid coffee drinker and subsequently exhibited heightened anxiety, due to the effects of Ciprofloxacin on caffeine. Additionally, he showed no improvement in symptoms after several days despite the antibiotics and returned to the hospital for further evaluation. An infectious disease specialist was consulted. The ID physician conducted several investigations and found the presence of Staphylococcus aureus in the patient’s blood work and suspected a possible lumbar spine infection. An MRI of the patient’s cervical and thoracic spines was ordered due to continued pain which now included neck and upper thoracic pain. The MRI of the cervical spine revealed an epidural abscess at C4-C6 levels requiring emergency surgery. After surgery the patient was ruled to be a permanent paraplegic.
Question(s) For Expert Witness
Would this patient have had a better overall prognosis if the infection was identified in a more timely manner and treated promptly?
Expert Witness Response E-005297
This case in very concerning and raises several questions. Firstly, what was the initial MRI targeting that the patient had performed? Was it of the cervical and thoracic spines? Or was it of his shoulder and neck? If imaging of the spine was not conducted that could have been a reason why the diagnosis was not made when the patient first began experiencing the symptoms. Secondly, why did the primary care physician suspect that the patient’s symptoms were caused by prostatitis? Was there an elevated white blood cell count, fever etc.? The patient’s history of presenting complaint does not suggest that this should have been in the differential diagnosis. Finally, what was done in the interim outside of the prostatitis treatment? Was the patient advised to come back for follow up in a few days? Based on the answers to these questions, I suspect more could have been done for this patient. It is strange that this went undiagnosed despite multiple visits to various health care providers. I also find if very odd that prostatitis was even considered as the culprit. The outcome for this patient could have been drastically better had the infection been diagnosed much sooner.
About the author
Dr. Faiza Jibril
Dr. Faiza Jibril has extensive clinical experience ranging from primary care in the United Kingdom, to pediatrics and child abuse prevention at Mount Sinai Hospital, to obstetrics in Cape Town, South Africa. Her post-graduate education centered on clinical research and medical ethics. Dr. Jibril is currently Head of Sales in the US and Canada for Chambers and Partners - a world leading legal ranking and insights intelligence company.