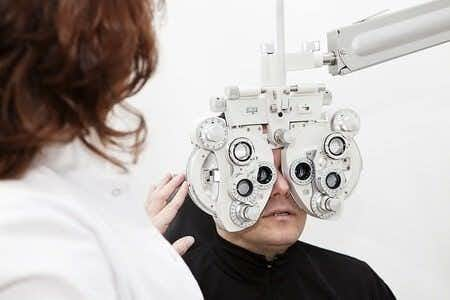
This case takes place in Pennsylvania and involves serious injuries to the Plaintiff’s eye following a routine surgical procedure. The Plaintiff, a female who worked as an air traffic controller, was scheduled to undergo an endoscopy to evaluate possible stomach bleeding. The patient, who had a previous medical history of degenerative eye disease which had required two cornea implants, asked the Defendant physicians how her eyes would be protected during the procedure, at which point the Defendants assured her that she would be fine. However, according to the surgical records, the patients eyes were only tapped during the procedure, rather than comprehensively protected by goggles. Additionally, records indicated that the patient was kept in a prone position during the procedure, and that no attempts were made to check or monitor the patient’s inter-ocular pressure. The patient was also given a number of drugs to facilitate the procedure, including Succinylcholine, which has been known to raise ocular pressure. When the patient awoke from the procedure, she immediately complained of serious pain in her right eye. It was observed that the globe and been ruptured, and that some of the eye’s vitreous contents had been expelled, with part of the patient’s original cornea implant protruding from the eye. An ophthalmologist who examined the patient observed that her vision was severely compromised, and emergency surgery was performed to repair the damage. Since the operation, the Plaintiff experienced multiple retina detachments, which resulted in the complete and permanent loss of vision in her right eye. As a result of these injuries, she is no longer able to perform her previous duties as an air traffic controller.
Question(s) For Expert Witness
1. Do you routinely treat patients similar to the one described in the case?
2. Are medications, such as Succinylcholine, known to result in increased intraocular pressure?
3. Could damage to the patient eyes been avoided had the patient been repositioned?
Expert Witness Response E-008300
This falls right within my expertise - open globe trauma is common and I have treated more than 70 cases in my career so far. I have many patients who have had corneal transplants, and I have performed both cataract and glaucoma surgeries on them. I have treated patients with a traumatic dehiscence of their transplant which typically involved severe blunt trauma. I have concern about the use of Succinylcholine in this case. There is some evidence and the classical teaching is to never use it in open globe trauma, however the coughing and bucking during intubation may be a bigger problem in this regard that made its use necessary. Both the lens and the iris move forward during use of succinylcholine, which may also have been a contributing factor in the poor results experienced by this patient. Additionally, proper positioning and protective padding is absolutely crucial to prevent injuries such as this. Dehiscence of corneal transplants require typically massive trauma, like that from a fist, heel, or table edge during a fall. The fact that the patient suffered this injury during her procedure suggests rather rough handling.
About the author
Joseph O'Neill
Joe has extensive experience in online journalism and technical writing across a range of legal topics, including personal injury, meidcal malpractice, mass torts, consumer litigation, commercial litigation, and more. Joe spent close to six years working at Expert Institute, finishing up his role here as Director of Marketing. He has considerable knowledge across an array of legal topics pertaining to expert witnesses. Currently, Joe servces as Owner and Demand Generation Consultant at LightSail Consulting.