A pathology expert witness advises on a case involving the delayed diagnosis of pancreatic cancer. Plaintiff was admitted to a Pittsburgh hospital because of abdominal pain and acute weight loss. He was diagnosed with biliary pancreatitis with possible pancreatic pseudocyst. A biopsy showed inflammatory tissue that was consistent with pancreatitis. A week later, a CT scan found gallstones, inflammation in the region of the gallbladder and pancreas and a cystic pancreatic mass that raised the possibility of pancreatic cancer. Another biopsy of the pancreatic mass showed inflammatory tissue and no evidence of malignancy. However, because of the possibility of the mass being pancreatic cancer, defendant doctors performed a cholecystectomy with cholangiogram, common bile duct exploration and both visual and tactile evaluation of the cystic pancreatic mass. The doctors concluded that the pancreatic mass was contained, inflammatory in nature, and consistent with benign pancreatitis rather than malignancy.
Because the pancreatic mass persisted, plaintiff eventually underwent an endoscopic ultrasound with transduodenal pancreatic biopsy, which disclosed adenocarcinoma. He subsequently had a Whipple procedure, nearly a year after his initial procedure. He underwent chemotherapy and remains disease free.
Plaintiff sued the defendant surgeons and the hospitals that performed the pathology examinations on grounds that their failure to diagnose his cancer during the initial surgery caused him to undergo the second surgery.
Question(s) For Expert Witness
1. What did the pathology tests show?
2. What type of tumor was this?
Expert Witness Response
I reviewed all the pathology slides and am in essential agreement with the diagnoses rendered. The needle aspiration and biopsy of the pancreatic mass performed in 2008 did not show any evidence of malignancy and the histologic findings were consistent with pancreatitis. The findings in the gallbladder were those of chronic cholecystitis and cholelithiasis. The Whipple resection performed in 2009 showed and intraductal papillary mucinous neoplasm (IPMN) with high- grade oncocytic morphology (which on the ultrasound guided aspiration cytology manifested features mimicking adenocarcinoma). There was no definitive evidence of invasive carcinoma in the resection specimen. All surgical resection margins and lymph nodes were free of tumor.
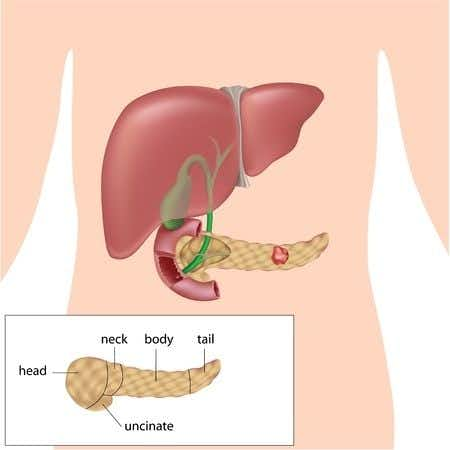
IPMN is a distinctive tumor, usually arising in the head of the pancreas, having a characteristic radiographic appearance. It is more common in males in their sixth and seventh decades of life and usually presents with non-specific symptoms. Some patients have a history of pancreatitis. It is relatively uncommon, accounting for 5% of pancreatic tumors. Because these tumors have potential to act in a malignant fashion, thorough sampling of the tumor for microscopic examination is essential to rule out areas of invasive carcinoma, as up to one-third of cases may exhibit evidence of malignancy (i.e. invasive carcinoma).
In this case, the tumor was entirely submitted for microscopic examination and there was no definitive evidence of invasive carcinoma. The tumor was characterized by its “oncocytic” appearance. This means that the cells had an eosinophilic (“oncocytic”) cytoplasm and nuclei with a prominent nucleolus. These oncocytic tumors tend to have high-grade dysplastic features. Despite its high-grade appearance, this recently described oncocytic variant of IPMN has not been shown to exhibit any difference in clinical behavior when compared to the usual, “garden variety” IPMN. However, if invasive carcinoma is detected in the oncocytic variant of IPMN, they tend to act in a less aggressive fashion, despite its high-grade cytologic appearance.
In summary, in 2008, the needle biopsy and aspiration of the pancreatic mass was not diagnostic for malignancy. Subsequent needle aspiration in 2009 yielded diagnostic cells and a subsequent Whipple procedure showed an IPMN that, while having a potential for malignant behavior if left untreated, did not have any evidence of malignancy, as defined by overt invasion into the fibrous capsule by atypical glands or single cells.
Patients (like plaintiff) who undergo a resection of an IPMN not associated with invasive carcinoma are considered to be “cured” of the tumor. However, because these tumors can be multifocal and may arise in branches of the pancreatic duct, routine follow-up is recommended as patients are at risk of developing a second tumor in the residual pancreatic tissue.
About the author
Kristin Casler
Kristin Casler is a seasoned legal writer and journalist with an extensive background in litigation news coverage. For 17 years, she served as the editor for LexisNexis Mealey’s litigation news monitor, a role that positioned her at the forefront of reporting on pivotal legal developments. Her expertise includes covering cases related to the Supreme Court's expert admissibility ruling in Daubert v. Merrell Dow Pharmaceuticals Inc., a critical area in both civil and criminal litigation concerning the challenges of 'junk science' testimony.
Kristin's work primarily involves reporting on a diverse range of legal subjects, with particular emphasis on cases in asbestos litigation, insurance, personal injury, antitrust, mortgage lending, and testimony issues in conviction cases. Her contributions as a journalist have been instrumental in providing in-depth, informed analysis on the evolving landscape of these complex legal areas. Her ability to dissect and communicate intricate legal proceedings and rulings makes her a valuable resource in the legal journalism field.