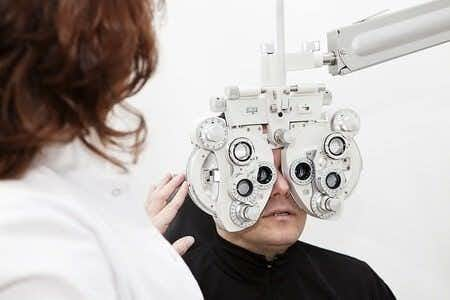
This visual impairment case involves a female patient in Nevada who came into the emergency room after experiencing nausea, vomiting, and severe weight loss. Though she was given medication to combat her nausea, doctors decided to order a CAT scan and have an extensive blood panel completed on the patient. However, her symptoms only worsened, even after being discharged from the emergency room entirely. After coming back to the emergency room again and again, consistently cleared and discharged by medical staff, the woman began to feel her arms become numb and constantly cold. She was admitted, once again, to the ER; after exhibiting symptoms of seizures and headaches, doctors decided to release her from the hospital once she could eat meals without vomiting. As the months passed, she began to go blind, with sharp, concentrated pain in the side of her head blurring her vision and causing her to consult an ophthalmologist. The doctor merely prescribed her some Moxifloxacin eye drops for what he thought was conjunctivitis. Weeks later, she lost her sight entirely. Doctors eventually concluded she had an autoimmune disorder, but the delayed diagnosis was detrimental to her standard of living and the patient was never able to fully recover from the ramifications of the late diagnosis.
Question(s) For Expert Witness
1. Do you routinely treat patients similar to the one described in the case?
2. Have you ever had a patient develop the outcome described in the case?
3. Do you believe this patient may have had a better outcome if the care rendered had been different?
Expert Witness Response E-009450
I routinely diagnose and treat patients with the specified disorder in a large academic medical center. My practice includes treating patients with optic neuritis, multiple sclerosis, neuromyelitis optica, and other optic neuropathies. I have seen several patients with severe vision loss due to optic neuritis that went on to develop MS or were subsequently found to have antibodies positive for neuromyelitis optica. It may be possible based on medical records that if an optic neuritis was diagnosed earlier with intravenous steroid treatment that the patient may have retained useful vision for a longer period of time. However, visual prognosis of NMO is very poor.
About the author
Joseph O'Neill
Joe has extensive experience in online journalism and technical writing across a range of legal topics, including personal injury, meidcal malpractice, mass torts, consumer litigation, commercial litigation, and more. Joe spent close to six years working at Expert Institute, finishing up his role here as Director of Marketing. He has considerable knowledge across an array of legal topics pertaining to expert witnesses. Currently, Joe servces as Owner and Demand Generation Consultant at LightSail Consulting.