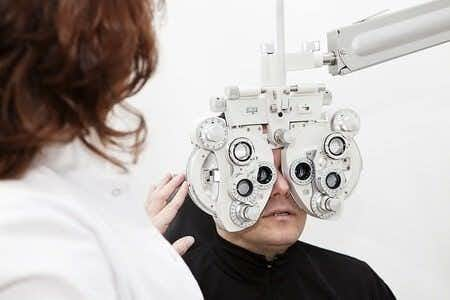
This case involves a female patient who suffered a retinal detachment after she was struck in the eye during a softball game. The patient underwent a repair procedure in the days following the injury, however the procedure was complicated by a suprachoroidal hemorrhage. The patient was discharged after the procedure with instructions to follow up should her vision deteriorate. A few days later, the patient returned to hospital reporting vision loss, pain, and redness. She was diagnosed with recurrent retinal detachment, and was told that she needed to wait for the return of her treating ophthalmologist to proceed with the procedure to reattach her retina. The procedure was performed a few days later, however the patient continued suffers from permanent vision loss, allegedly due to the delay she experienced before undergoing surgery.
Question(s) For Expert Witness
1. Do you routinely perform retinal detachment repairs?
2. Can you speak to complications that can occur during retinal detachment repair, such as a suprachoroidal hemorrhage?
3. Are you familiar with patients who have recurrent retinal detachment?
4. Can you speak to the correlation between timely repair of retinal detachment and long term side effects, such as vision loss?
Expert Witness Response E-009450
I routinely treat patients with rhegmatogenous and complex retinal detachments. The success rate of retinal reattachment varies from approximately 60-90% depending on the anatomical features of the presenting detachment. I am able to definitively speak to complications that occur during retinal detachment repair including suprachoroidal hemorrhages, recurrent detachment, and proliferative vitreoretinopathy. Depending on the configuration of the retinal detachment, there are guidelines to how quickly a repair should be done, and it seems like the delay experienced here was a critical factor in the patient's vision loss. I am a faculty member at a major university medical center which has a highly competitive ophthalmology residency and vitreoretinal surgery fellowship. I am involved in resident/fellowship training in the clinic and operating room on a daily basis. I am a fellowship trained, board certified vitreoretinal surgeon and have performing retinal detachment repairs for the past 6 years. My surgical approach utilizes state-of-the art sutureless 25-gauge vitrectomy surgery which is often combined with scleral buckling depending on the retinal configuration. With these techniques, I have successfully repaired first time detachment, recurrent detachment, and complex detachments due to proliferative vitreoretinopathy and diabetic retinopathy. I also teach residents and fellows techniques in vitreoretinal surgery through hands-on experience in the operating room and through lectures. Lastly, I am an NIH funded physician-scientist specializing in vitreoretinal biology and disease and have a full-time laboratory investigating molecular mechanisms of cells death in the retina.
About the author
Joseph O'Neill
Joe has extensive experience in online journalism and technical writing across a range of legal topics, including personal injury, meidcal malpractice, mass torts, consumer litigation, commercial litigation, and more. Joe spent close to six years working at Expert Institute, finishing up his role here as Director of Marketing. He has considerable knowledge across an array of legal topics pertaining to expert witnesses. Currently, Joe servces as Owner and Demand Generation Consultant at LightSail Consulting.