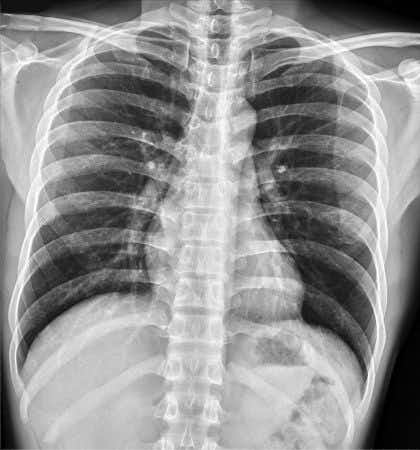
This case involves a thirty-five-year-old female who presented to her neurologist with difficulties swallowing. Her past medical history included myasthenia gravis and hypertension. She first established care with her neurologist when she was diagnosed with myasthenia gravis, an autoimmune neuromuscular disease. Based on these findings, the neurologist believed that she experienced an exacerbation of myasthenia gravis. He increased the dosage of her medication, pyridostigmine, despite the fact that she was not having any other symptoms. He then scheduled her for a one-month, follow-up appointment. Over the next month, she developed chest pain, shortness of breath, cough, and facial plethora which caused her to go to the hospital. At the ER, a CT scan was performed which revealed an anterior mediastinal mass. Biopsy confirmed that the woman had a stage III thymoma and was scheduled for a thymectomy. After surgery, she required months of radiotherapy and chemotherapy. One of the chemotherapy agents used to treat her condition was doxorubicin. Six months after chemotherapy, the woman’s ejection fraction was 25%. She was diagnosed with a dilated cardiomyopathy secondary to doxorubicin therapy. Between receiving chemotherapy for her thymoma and managing her cardiomyopathy, the patient experienced prolonged hospitalizations and pain.
Question(s) For Expert Witness
1. Did the neurologist properly identify the patient’s condition in this case, what could have been done to treat this woman’s condition?
Expert Witness Response
The neurologist, in this case, did not identify a condition that is seen in 10--15% of patients with myasthenia gravis (MG). Instead, he thought that she was experiencing symptoms of MG and increased her medication dosage. Thymoma is an epithelial cell tumor of the thymus located in the anterior mediastinum. Due to its location, a thymoma can present as difficulties swallowing due to compression of the esophagus. It can also compress the superior vena cava causing dyspnea, headache, edema, venous distention, lightheadedness, cough, and facial redness. Thymoma is also associated with pure red cell aplasia and other autoimmune diseases. Thymoma is typically diagnosed with a CT scan, which reveals a lesion in the anterior mediastinum. Needle biopsy is also performed under CT guidance. Laboratory work can assist with the diagnosis using a full blood count, protein electrophoresis, electrolytes, liver enzymes, and renal function. Surgery is the most successful intervention for a thymoma. For all stages, a thymectomy should be performed. Stage III and IV disease may also require radiotherapy and chemotherapy. A common chemotherapeutic used to treat thymoma is doxorubicin. Dilated cardiomyopathy is a major side effect of doxorubicin use. Had the diagnosis been made earlier during stage I or II, she would not have required chemotherapy.
About the author
Jason Cohn
Jason is a 4th year medical student pursuing a career in Otolaryngology/Facial Plastic Surgery. His Interest include sports, fitness, chemistry, otolaryngology, plastic surgery, allergy/immunology, surgical oncology, human genetics, public health, preventative medicine, and rheumatology.